News
- NEW Best Treatment Guidelines for Seizures
- Diagnostic procedures
- Epilepsy surgery
- Epilepsy in Special Populations
NEW Best Treatment
Guidelines for Seizures
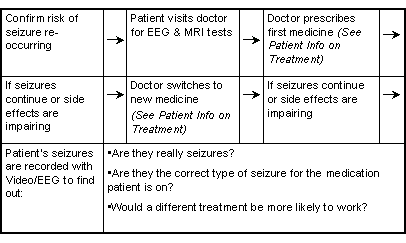
Patients and their families may sometimes feel the approach to their care is not part of a well-structured plan. The outline here shows the recommendations of experts in seizure management. The professional organizations of these physicians have published these strategies in various forums. Patients and their families should expect these steps from their physicians if the best level of care is to be maintained.
Sometimes patients may wish to not accept these recommendations but these strategies are based on evidence and treatment trials. These are the pathways that help the largest number of patients and are therefore most advisable.
[ top of page ]
Diagnostic procedures
 The description of their seizures and the medical history of the patient are used to determine that epilepsy is a possibility. There is no test that is always abnormal in determining seizures, but there are several tests that look at pictures of the brain and can be helpful.
The description of their seizures and the medical history of the patient are used to determine that epilepsy is a possibility. There is no test that is always abnormal in determining seizures, but there are several tests that look at pictures of the brain and can be helpful.
Computerized tomography (CT) is of limited use as it is not very sensitive in finding abnormalities. CT is often done to exclude significant problems first, but magnetic resonance imaging (MRI) sees the brain much better. Small tumors, abnormalities in the brain's shape or blood vessels, and scars from head injury are seen much better and make MRI mandatory where a seizure could be caused by these conditions.
Electroencephalography (EEG), or brainwave recordings, tell us how the brain is working. There are normal EEG waves and others that suggest injury or the risk for seizures. There are different EEG abnormalities for different types of seizures.
The problem with testing is that the majority of MRIs and EEGs are normal in people with seizures and epilepsy, so having normal test results is likely. Normal results can be upsetting, as many patients then want to know how we can be sure of the diagnosis. Normal results are positive, as the chance that the seizures are less troublesome and medications can be discontinued in the future is better. More testing will be done if the seizures are hard to stop but initially these might not be helpful.
[ top of page ]Epilepsy surgery
The seizures most likely not to stop with medications are the partial seizures. They begin in a small area and spread to involve other parts of the brain. Partial seizures can be stopped if the area they start in can be surgically removed. Fortunately, the brain can allow such removals, because it has several areas involved in the same activity and removing one area does not reduce the person's ability to do things.
For instance, memory is stored in the temporal lobes on both sides. Removing the temporal lobe that is causing continued seizures will result in the remaining temporal lobe doing the memory activity. The brain has many of these duplicate or redundant functions. Surgically removing the epilepsy area can allow many people to have seizure-free lives and many can reduce or discontinue their medicines. Rates of seizure freedom vary from 50-70% by location of the seizure's starting area. Complications such as reduced functioning ability, bleeding or infection occur in 1-4% of patients, according to several research articles.
What is functional brain mapping?
Seizures beginning in the area of motor, sensory or language function are clinically mapped using stimulation mapping. Mapping is performed by stimulating the brain at low electrical current and mapping the appearance of a localized muscle jerk or loss of higher cortical function. This mapping can be performed intraoperatively (during surgery) with an awake patient or extraoperatively with sheets of grid electrodes. The seizure may begin in a crucial area of brain function and surgery may not be recommended. Fortunately, this is not a common occurrence.
How can neuropsychology help with surgery?
Neuropsychology can localize an area of functional loss in the brain. This area of dysfunction is strongly correlated in epilepsy with the area of seizure onset. Functions such as memory have verbal and nonverbal components that can be separated out along language-dominant and non-dominant hemispheres of the brain.
The protocol used for confirmation of seizure onset incorporates neuropsychological results. Most epilepsy centers have found that with testing they can also predict memory difficulties before surgery on the temporal lobe and therefore modify the surgical procedure to prevent amnesia. Selection of appropriate tests in the neuropsychological test battery is crucial for its success. The interpretation is very dependent on familiarity with prior results in epilepsy patients.
What makes uncontrolled epilepsy severe enough to consider a surgical treatment?Alternative therapy, including vagus nerve stimulation and epilepsy surgery, should be reserved for those patients continuing to have seizures despite the use of standard medications. If medications work, then invasive procedures are not an appropriate treatment.
Persistent, continuing seizures may be perceived as non-threatening to the patient, but seizures do restrict patient freedom and increase risk of injury. Alternative treatment, like surgery, may not be an option if the severity of the patient's limitations are too difficult to appreciate. Seizures should not be allowed to restrict a patient's life when he or she might be seizure-free with a surgical treatment.
If epilepsy comes from a scar, then how can trading one scar for another reduce seizures?The concept of the epilepsy scar or gliosis is a reasonable way to explain the cause of epilepsy to a patient, but gliosis does not produce seizures. Damaged neurons produce seizures. These epileptic cells form the epileptic focus that may or may not be structurally different from surrounding tissue.
The process of surgical incision is a different process. When the cortex of the brain is divided by incision, the line of injury is well demarcated and neurons are either transected or unaffected. Little damage occurs in the controlled environment of epilepsy surgery to produce new, injured neurons. Hence, the cause of epilepsy is removed without producing a new cause. A surgical treatment of epilepsy works very well.
Can routine EEG pick the good surgery candidate?
Routine electroencephalography (EEG) can be a useful tool in classifying a patient's seizure syndrome. Some seizure manifestations are typical for seizure onset in the temporal, frontal, parietal or occipital cortex. Specific electrical discharges from these areas can help determine where seizures originate.
Unfortunately, EEG is limited by the amount of time that can be sampled. The prevalence of any specific abnormal discharge is difficult to estimate from standard EEG. Prolonged recordings can estimate the ratios of certain discharges and predominance to help localize seizure onset when accompanied by video-EEG monitoring. Patients who have abnormalities on both sides of the brain, according to the EEG, may still be candidates for surgery. Video-EEG monitoring can record all the patient's typical seizure manifestations. If the recordings all have unilateral onset, then surgery may be successful.
What makes this brain surgery different?
Many patients have been personally touched or are familiar with someone who has had a craniotomy and believe that paralysis or speech difficulty are the only outcomes from craniotomy. They are frequently unaware or don't realize that an initial, life-threatening cause, such as a cancerous tumor or collection of blood between the layers of membranes covering the brain, leads to that craniotomy.
Surgery as a treatment of epilepsy is not usually viewed as life-saving. This fact places the responsibility on the evaluators to avoid high-risk surgeries that could cause unwanted damage to the brain. The morbidity of these surgeries is about 5%. The evaluation process helps define and explain to the patient the risks involved. Neuropsychological tests help predict patients at risk for amnesia.
The Wada test (unilateral intracarotid sodium amobarbital test), produces temporary hemispheric anesthesia and allows testing of memory in the opposite hemisphere. Functional brain mapping can also assist in preventing deficits following surgery.
Is surgery for epilepsy always possible?
Not all patients whose seizures are resistant to medical therapy can be helped by surgery. The involvement of functionally important brain areas or the bilateral condition of seizure onset often precludes a surgical treatment. It should be reiterated that these decisions are not often discernible before monitoring, and many initial assumptions concerning the suitability of a patient for surgery may be erroneous. Trials of newer anti-epileptic medications are available to patients where surgery is unavailable.
Epilepsy in Special Populations
When treating children with epilepsy, it is important to remember that they are not simply "small adults." They need special attention to the type of seizures they have and the medications that are best suited for them. Children's developing brains can be affected by some epilepsy medications, which is unique to a child. School performance is a measure of this effect as are a child's interaction with others and the development of his or her social skills.
Children are affected in different ways by medication. Sedating medication in adults often leads to behavior outbursts in children. Phenobarbitol sometimes produces a "monster child" and such an effect must be monitored for from all medications. In addition, children often need higher doses of medications because their bodies eliminate the medicines faster.
Maturing Americans, that ever-increasing number of people eligible for AARP, have important needs as well. Seizures and epilepsy are so frequently associated with the young that people fail to note that the highest frequency is in individuals over age 65. The frequency of stroke and the damage it creates is mostly responsible for this higher rate.
Best estimates are that 2-3% of those over 65 have seizures. Older people's bodies eliminate medications slower than youngsters and must often have medication adjustments done more slowly using lower doses to avoid side effects. According to the State of Minnesota, older individuals take an average of eight medications each. Seizure medications were among those most frequently prescribed.
[ top of page ]